Designing adaptable healthcare spaces
How innovative spatial design has helped transform care at a London eye hospital

As the COVID-19 pandemic took hold, the challenges facing the UK national health service (NHS) multiplied.
In addition to dealing with the immediate effects of the virus, hospitals and clinicians struggled against restrictive measures that slowed routine services – such as ophthalmology – to a crawl.
By 2021, the devastating effects were apparent:
- A 23% reduction in eye test delivery during 2020 – 4.3 million less tests than in 2019
- 235,000 necessary eye surgeries missed or delayed
- 2,986 estimated cases of avoidable blindness and vision loss, purely due to delayed diagnosis and treatment of eye disease
With no more time to waste, a multidisciplinary team of researchers from UCL was commissioned by the National Institute for Health and Care Research (NIHR) to find new ways to reduce the backlog at Moorfields Eye Hospital in London.
Looking for the safest shortcuts
Grant Mills, Professor of Healthcare Infrastructure Delivery at the Bartlett School of Sustainable Construction, outlined the goals of the project and discussed the challenges they faced.
“The aim was to design a swift and even patient flow - one that required fewer waiting rooms, patients spending less time in a health care facility, and the combination of diagnostics tests for more efficient clinician review.
“So we’re looking for ways to get the patients in to get lots of tests together (combining diagnostics for glaucoma, retina and cataract care), which shortens the time for results to be batched and sent to the clinician.”
Grant is keen to stress that the project’s clinical leaders always viewed these efficiencies through a lens of improving care standards.
“It was about adapting around that patient-technician interaction – it's so, so important, we saw that over and over again. Technicians building a strong relationship face-to-face with the patient.
“But there were challenges around combining three different clinical areas, all with different technologies.
“There were challenges from bringing together academics from different domains to gather evidence.
“And of course, with 5,000 patients – some of whom potentially had Covid – moving through a space there were huge operational challenges, too.”
As the crisis deepened, the need for tangible results drove a more radical approach to healthcare planning.
“They’re trying to have a swift and even patient flow - one that required fewer waiting rooms, patients spending less time in a health care facility, and the combination of diagnostics tests for more efficient clinician review.”

Shining a light on outdated approaches
The case for a new approach was strengthened by the absence of any meaningful design guidance. Healthcare architect and senior research fellow at the Bartlett School of Construction, Dr Anne Symons said:
“The design guidance is from 1990. It’s so old, it’s actually not supposed to be used, but if there’s nothing else, people will use it. The pandemic released us from that and allowed us to do something quite different.”
Looking to implement a data-led approach, Duncan Wilson, Professor of Connected Environments and Connected Environments MSc Programme Director at the Bartlett Centre for Advanced Spatial Analysis, was tasked with devising the project’s data capture methodology.
“We needed the evidence to convince the clinicians to bring them on board with a new way of doing things.”
“The design guidance is so old... but the pandemic released us from that and allowed us to do something quite different.”

A new perspective on healthcare spaces
Their first step was to assess the suitability of the existing facilities at Moorfields Eye Hospital.
Professor Peter Scully from the Bartlett School of Architecture explains:
“As we began to look at the hospital, we asked, ‘what are the things that only the hospital space can provide? Are there things taking up valuable hospital space that could be done in other spaces?”
These questions also helped the team identify ways that the current environment was negatively impacting diagnostic efficiency.
“In the hospital settings, it’s very much stop-start,” Anne Symons explains.
“There’s no flow. You’d go to a waiting room to begin with, and you’d do the first bit, then go to another waiting room to do the next bit, then another one after that.
“The machines wouldn’t be collected together, they’d be scattered into small rooms. And it’s not easy to track patients in these conditions.
“So this was a real opportunity to see the flow of patients, and to speed it up”.

The key factor was adaptability.
The new diagnostic hub didn’t need to meet the strict requirements of a treatment or surgical setting. It had to allow rapid reconfigurations of walls, furniture and equipment, as the team analysed the data and tested new iterations of the ideal diagnostic space.
And one kind of location stood out as being uniquely suited to these conditions: retail space.
As Duncan says, “the beauty of the retail outlet is that it’s designed for fit out. Retailers change the displays every season – so they design spaces to be shifted around and changed every eight weeks, because that’s what their business model relies upon.”
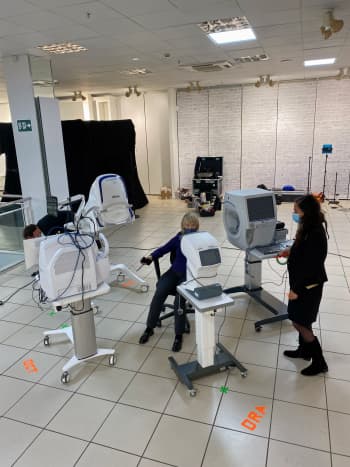
The new diagnostic hub was created in a retail unit at the Brent Cross Shopping Centre, nine miles from Moorfields.
A bigger picture, drawn with data
Data from 17 Ubisense Ultra Wide Band (UWB) sensors was used to identify and track the movement of individuals within the new diagnostic hub. This data was then combined with environmental measurements from air samplers located throughout the clinic.
By measuring temperature, humidity, CO2 concentrations and particulate loading, a sophisticated dataset was created that allowed the research team to assess the speed and safety of virtually every aspect of the diagnostic process.
Across the four iterations of the environment, the data proved instrumental in identifying flawed logic and assumptions about the design requirements. As Duncan explained:
“These spaces are laid out with machines and flows, and there’s design logic behind them. But then ‘the grit’ enters the system – the people. And people adapt and find better ways to do things.
“One example we saw was a space with good sight lines, that was theoretically more accessible. But when they got there, the clinicians used the one next door instead.
“And when they explained why, it was so obvious – they used the one next door because it was less visible, because it had less sight-lines and visibility. And now we had the data there to support it.”
The data has proved so useful, there are now plans to permanently install sensors in some healthcare settings to continuously monitor the usage of spaces and provide performance data.
“These spaces are laid out with machines and flows, and there’s design logic behind them. But then ‘the grit’ enters the system – the people. And people adapt and find better ways to do things.”

A vision of the future of healthcare
While the team are careful to point out that the project was one of several measures implemented by Moorfields to speed up diagnosis, the overall result has been very successful. For nearly all of the diagnostic specialisms, the time taken to assess each patient has been reduced significantly.
“We’re at the beginning of a transformation which requires healthcare designers to quickly adapt to incorporate changing technology and innovative clinical care pathways. This will see us designing new community settings,” said Grant.
“There are a lot of opportunities now to extend the diagnostic clinic in new real estate situations. I don’t think we can claim it’s a first – Moorfields was already a very networked hospital that already delivers from 22 different sites and locations.
“But the way we did it was quite unique, in terms of gathering the evidence to support this distributed model and creating a flexible kit of parts to use in open plan situations.
“I think it shows how we could work more closely with our NHS partners to help improve efficiency.”
Peter is keen to point out the renewed importance in a post-COVID world of designing for change in healthcare.
“One of the things we know is going to happen is change. Given what’s happened to healthcare perspectives just over the last three years, the idea that we could sit here today and plan for how a space was going to be used for healthcare delivery in ten years' time seems fairly preposterous.
“We need healthcare spaces that are capable of adapting to the needs of the time.”
“One of the things we know is going to happen is change. We need healthcare spaces that are capable of adapting to the needs of the time.”

About the authors
Professor Duncan Wilson
Professor of Connected Environments, the Bartlett Centre for Advanced Spatial Analysis, UCL
Professor Peter Scully
Professorial Research Fellow, the Bartlett School of Architecture, UCL
Connected Environments Lab, the Bartlett Centre for Advanced Spatial Analysis, UCL
Connected Environments Lab, the Bartlett Centre for Advanced Spatial Analysis, UCL
Find out more about the Connected Environments MSc
This Master's programme teaches skills in connected environment technologies, interlinking the Internet of Things (IoT), Artificial Intelligence, (AI), Virtual Reality (VR) and Data Science, enabling students to gain hands-on experience of electronics, programming and the design process.
Story produced by All Things Words
© UCL The Bartlett 2023